The Woolcock Institute of Medical Research
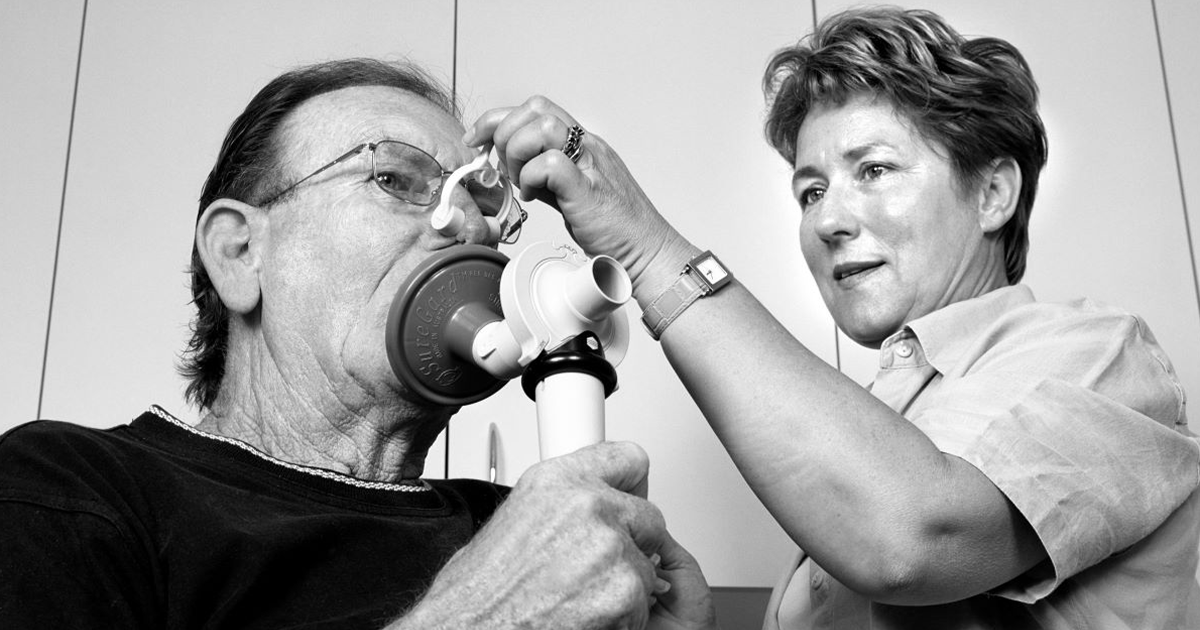
Asthma care: Living in the past?
Asthma researchers and scientists are increasingly voicing their concern that outdated government regulations and health initiatives are impacting asthma care in Australia at a time when it should be getting better.
Current treatments and best practice guidelines mean most people with asthma can live symptom free, with no limit on their level of activity, no night waking, no airway obstruction and no exacerbations while needing their reliever medication less than twice per week.
For many, though, that is not the case. Asthma care in Australia is getting worse because new strategies to treat the disease and not just alleviate the symptoms are not being used consistently. And asthma care is also deteriorating because of a general view in the community that asthma is something that can be lived with and not a disease which requires a management plan involving comprehensive assessment, regular review and treatment adjustment.
Asthma was listed as a National Health Priority in the early 2000s in response to high mortality rates. Prior to this, when mortality rates were high, short-acting beta agonist (SABA) relievers were made available “over the counter” at pharmacies for emergency use. Contrary to the intention and best practice, they became, and continue to be for some patients, the default option. Current prescribing regulations mean that people can get up to 12 inhalers every six months from the pharmacy without seeing their GP. The consequent underuse of newer, safe and effective medications has also led to an increase in prescriptions for oral corticosteroids to manage flare-ups.
While this strategy did reduce the number of deaths, Woolcock alumnus Professor Christine Jenkins argues that we are now locked into an “asthma echo chamber” that is long past its use-by date.
“Over-the-counter SABA availability is antiquated and harmful. Oral corticosteroids are overused which may lead to long-term cardiovascular and metabolic harms, newer treatments are under-used and we are not implementing simple evidence-based care that we know prevents symptoms and exacerbations,” she says.
The current Global Initiative for Asthma (GINA) guidelines recommend assessment of asthma triggers, diagnostic spirometry, individualised action plans, combined reliever/preventer medication and education on device use and adherence.
However, almost 40 percent of people with asthma in Australia still rely on SABA reliever medication alone.
“We need to upend SABA as the first treatment for asthma and treat asthma in a proactive, comprehensive way,” she says.
One of the obstacles to that is the requirement for an Authority script for internationally recognised first-line treatment with combination inhaled corticosteroid /fast-onset long-acting beta agonist under Australia’s Pharmaceutical Benefits Scheme.
Want to stay up to date with our research on sleep and respiratory conditions?
Sign up to our monthly newsletter
While in practice in primary care this doesn’t present a significant impediment it “creates the idea that this treatment isn’t safe in some way, that it’s a dangerous treatment which can only be prescribed on Authority. It creates bad vibes for both practitioners and patients,” says Jenkins. “While in fact, this is a highly effective treatment for at least half of the asthma population in Australia.”
According to the GINA Pocket Guide, the next step for those who are still symptomatic is Maintenance and Reliever Therapy.
The Woolcock Institute of Medical Research’s Executive Director, Professor Carol Armour agrees.
“We need to move from a rescue culture in asthma which is reliant on relievers, to a prevention culture which is proven and has been recommended for more than a decade. We need people to know that things have changed,” she says.
Good asthma management requires comprehensive assessment, adjustment, regular review and the advice of your healthcare provider though. This is challenging under the current system where GPs are time-starved and, more often than not, limited by 15-minute consultation slots.
The “quick-fix solutions” currently relied on by many people with asthma are not serving them or our health budget well. New preventer and reliever treatments managed in partnership with health providers offer a way to better control their asthma and breathe more easily.
Find out more
Sleepwalking towards more harm from asthma, Medical Journal of Australia
OTC SABA is 'antiquated and harmful', thelimbic










